U.S. News & World Report – Health
5 Things to Know About Prostate Cancer
S. Adam Ramin, M.D., U.S. News & World Report January 9, 2019
Those of us in the medical profession are faced with a dilemma when educating the public about diseases: We need to inform — without creating hysteria. That’s tough to do today; sometimes it’s the less reputable voices that become the loudest, and we begin hearing from patients who “read somewhere” that XYZ condition is caused by “doing something completely normal that basically everyone does.” Misinformation is the last thing we need because it clouds the truth. And sometimes, changing the way information is delivered can go a long way toward creating understanding and equipping people with the facts to make the best, most informed health decisions. Prostate cancer is one of those conditions surrounded by some reasonably widespread misinformation, and this is an excellent place to help clear it up.
Most people know that prostate cancer is a disease that affects only men, since the prostate gland is one part of the male genital/urinary system. But did you also know that it’s the second leading cause of cancer death in men, just behind lung cancer? Shocking statistics aside, prostate cancer is not a death sentence for many of the men who develop it. In fact, most men who are diagnosed with prostate cancer don’t die from the disease. And in even better news, the trend in death rates among men diagnosed with prostate cancer has been steadily declining since the mid-1990’s, according to the American Cancer Society. We can thank better education, diagnosis and treatment options for that.
[See: What Only Your Partner Knows About Your Health.]
Prostate cancer isn’t a disease that just affects “old guys.” With humans living longer on this earth than ever before, does 66 seem “old” to you? Your answer to that question is likely relative to how close you are to that age. But, the average age of prostate cancer diagnosis for men is in the mid-60’s range, and I can say from experience that the men in this age range (and younger) who I’ve delivered a diagnosis to didn’t feel “old enough” to receive it.
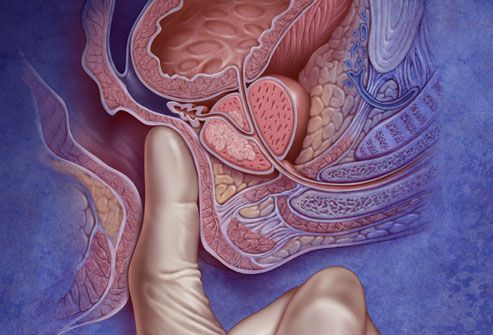
Speaking of diagnosis, one valuable tool that helps uncover prostate cancer is something called a PSA test. PSA stands for prostate-specific antigen. This is the protein produced by the prostate gland that can be a prostate cancer indicator depending on the levels or velocity of the protein in the bloodstream. However, a PSA test really isn’t a “cancer test.” There are some issues besides cancer that can result in an elevated PSA level in a man, from inflammation to infection, and this test alone isn’t a definitive prostate cancer detector. Instead, it can be a first step in further evaluating a potential problem. If a physician is concerned with a man’s PSA levels and suspects prostate cancer, he or she would then move to more definitive diagnostic measures, including a biopsy of the prostate.
[See: 10 Things Younger Men Should Know About Prostate Cancer.]
Regarding what causes prostate cancer, research has currently not revealed a direct cause, and a vast array of misinformation remains out there. For example, it was once suspected that having a vasectomy increased a man’s risk for developing prostate cancer. This topic has been researched heavily, and there is currently no reputable clinical evidence to prove it. Frequent ejaculation was also previously believed to cause prostate cancer, but this has been debunked by science, especially now that some research is revealing that more frequent ejaculation is associated with a lower prostate cancer risk.
What is known is that there are vital factors that can increase prostate cancer risk. Beyond the age factor, these include:
— Genetics/family history (having a first-generation relative who has been diagnosed with the disease).
— Race and ethnicity (African-American men and men of African ancestry are at a higher risk than other races).
— Geographic location (prostate cancer is most common in North America).
When it comes to the treatment of prostate cancer, we again see varying schools of expert thought, and all have merit. Some medical experts believe that treating a cancer that won’t likely result in death isn’t the best course of action. However, we can’t always know when a prostate cancer that starts out as “slow growing” may turn aggressive. And from a personal decision standpoint, there are plenty of men who don’t sit well with knowing they have cancer, but have been told not to do anything about it — yet. These factors and plenty of others make the treatment decision a very personal one and require the thoughtful consult with loved ones and a trusted physician who can help make the treatment decision that’s right for you or the man you love. There really is no one-size-fits-all option here.
[See: 10 Lessons From Empowered Patients.]
So the next time you read a headline about prostate cancer (or any other medical condition, for that matter) that has you shocked and are wondering whether or not it’s true, consider the source. Has it been distributed by a reputable news outlet? Was it written by a medical expert who has authority, credentials and experience in the diagnosis and treatment of the condition being discussed? Is the article attempting to persuade you or a loved one into buying a product or service intended to “cure” the disease? Figuring out the answers to these questions can go a long way toward helping you figure out what’s true and what isn’t. And when in doubt, call your doctor.
S. Adam Ramin, M.D., is a board-certified urologist and founder and medical director of Urology Cancer Specialists in Los Angeles. He is a medical staff member at prestigious medical centers such as City of Hope National Medical Center, in Duarte, California, where he has served as Assistant Professor of Surgery in the Department of Urologic Oncology, and Cedars-Sinai Medical Center in Los Angeles, where he performs robotic laparoscopic prostatectomy.
Dr. Ramin received his Bachelor of Science degree in 1990 from the University of California, Los Angeles, with a double-major in biochemistry and philosophy. He went on to complete postgraduate training with an internship and residencies in general surgery and urology at Loma Linda University in Loma Linda, California. He performed his fellowship training in urological oncology at the City of Hope Medical Center in Duarte, California. Upon completing his extensive medical education and training, Dr. Ramin established his private medical practice in the Los Angeles area. He became a contributor to U.S. News in 2017, covering a range of prostate cancer, urologic cancer and urological health-related topics. As an expert in prostate cancer and robotic laparoscopic prostatectomy, Dr. Ramin has published numerous textbook chapters, peer-reviewed articles, abstracts and presentations on prostate cancer and urological health subjects. He is certified by the American Board of Urology in Robotic Assisted Urologic Surgery and Urologic and Oncology and Laparoscopic Surgery, and he has trained numerous urologists in techniques of minimally invasive laparoscopy and robotic surgery. Dr. Ramin is a past president of the Los Angeles Urological Society and is a member of numerous professional medical societies including The American Urological Association, American Medical Association and American Society of Laparoscopic Surgeons. Dr. Ramin is a frequent medical expert contributor to mainstream media publications and news outlets, including local ABC and Fox television affiliates, as well as national online publications such as MSN, Yahoo, Women’s Health, Men’s Health, Huffington Post and Reuters Health.
